Total knee replacement surgery, also called total knee arthroplasty, is most often performed to relieve severe pain in patients who have not experienced relief with conservative treatment. Besides pain relief, knee replacement can help restore function in severely damaged knee joints.
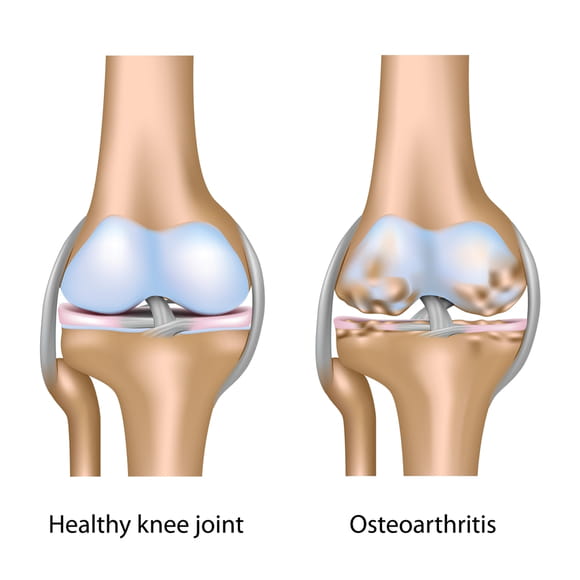
Osteoarthritis is the most common form of arthritis of the knee, causing severe knee pain, swelling and inflammation. Knee arthritis can cause problems with daily life activities, such as walking, climbing up and down stairs, bending and getting in and out of chairs. Some people also have knee pain at rest, interfering with sleep.
Anatomy of the Knee Joint
The knee, like the elbow, is what’s known as a hinge joint, as opposed to a ball-and-socket joint such as the hip or shoulder. The knee is a meeting of three bones: the lower leg (the tibia, or shin bone), the thigh bone (femur) and the kneecap (patella).
Wrapping the ends of the tibia and femur is articular cartilage. This smooth tissue enables the bones of all joints to glide together smoothly and prevent bone-on-bone contact. This is the tissue that becomes damaged due to osteoarthritis; in end-stage osteoarthritis, the articular cartilage is all but gone and the tibia and femur are riddled with bone spurs (also known as osteophytes).
 The underside of the patella is also lined with cartilage, which often becomes damaged due to wear and tear, injury, misalignment or muscle imbalances drawing it off its track.
The underside of the patella is also lined with cartilage, which often becomes damaged due to wear and tear, injury, misalignment or muscle imbalances drawing it off its track.
Also around the knee are a number of ligaments holding bones together and tendons attaching muscles to bone. The knee has four main ligaments:
- Anterior cruciate ligament (ACL)
- Posterior cruciate ligament (PCL)
- Medial collateral ligament (MCL)
- Lateral collateral ligament (LCL)
Tendons insert at the knee bones and hold muscles in place, such as the:
- Calf muscles
- Quadriceps
- Hamstrings
Procedure
The term “knee replacement” is actually somewhat misleading. After a total knee replacement, most of the original knee anatomy will still be in place. The majority of the tissue to be replaced is cartilage, along with some damaged bone.
A total knee replacement procedure requires anesthesia – typically a spinal, which blocks pain below the waist and allows the patient to sleep through the surgery. An intravenous antibiotic will be administered before, during and after the procedure to help prevent post-surgical infection. A nerve block around the knee will also be given to numb it, which can last up to 3 days after the procedure.
The knee is placed in a bent position to expose all surfaces of the joint. A small incision is made and the kneecap is moved aside to expose the joint. In a total knee replacement surgery, all three compartments of the knee are replaced:
- Medial (inside)
- Lateral (outside)
- Patellofemoral (front)
In some cases, only one of these compartments are damaged, so surgeons might perform a partial knee replacement, also known as a unicompartmental replacement.
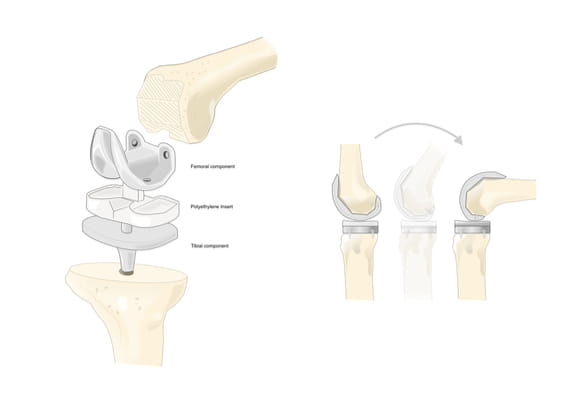
The surgeon removes the damaged portions of the bones at the thigh bone (femur) and the top of the shin bone (tibia) and replaces them with a prosthetic device – an artificial joint – made of plastic and a metal alloy. The back of the kneecap is resurfaced with a plastic button.
 UOA uses computer navigation and MRI-based custom cutting blocks. These tools help the surgeon place the implants in the proper position and alignment. Using these advanced tools helps ensure a good outcome for the procedure, as well as maximize longevity for the prosthesis.
UOA uses computer navigation and MRI-based custom cutting blocks. These tools help the surgeon place the implants in the proper position and alignment. Using these advanced tools helps ensure a good outcome for the procedure, as well as maximize longevity for the prosthesis.
Before closing the incision, the new knee is bent and rotated to ensure proper function. The surgery takes approximately 60 to 90 minutes.
Knee Replacement Outcomes
Total knee replacements are well documented to improve quality of life for people with knee arthritis. A knee replacement can potentially allow those who have had the surgery to take part in activities they’ve had to give up when their arthritis became debilitating.
A small study published in Arthritis Care and Research examined more than 50 patients who had a total knee replacement. Researchers measured metrics related to physical activity and quality of life. After 12 months, physical activity markedly improved and patients reported a higher quality of life.
Furthermore, patients are usually satisfied with their knee surgeries, but it’s important to keep expectations realistic. A 2016 study published in Knee Surgery and Related Research suggests that a total knee replacement produces high patient satisfaction scores, but those scores are lowered when expectations are not met.
Surgeons should communicate clearly the risks, benefits and recovery timeline before surgery. Patients are encouraged to listen carefully, ask questions and set realistic expectations.
Knee Replacement Recovery
Recovery in the Hospital
Knee replacement requires pre-surgical preparations and subsequent physical therapy. A hospital stay of one to two days is typical, though some patients are able to go home the same day. Many of the total knee replacements we perform at UOA are able to be done on an outpatient basis, no hospital stay necessary.
Though pain and discomfort will be present, walking the same day as surgery is paramount. A walker, cane or other assistive device may be used for support and will be required after release from the hospital. UOA surgeons routinely use peripheral nerve blocks during surgery to reduce pain and the need for opioid-based pain management.
Exercises that are performed while in the hospital will be prescribed with a home therapist. Outpatient physical therapy will also be prescribed and usually begins within a couple weeks after surgery. Physical therapy is vital to restore knee strength, improve knee range of motion, reduce scar tissue and to wean off the use of assistive walking devices.
Getting Back to Daily Activities
Staying active after returning home is a key component to recovery; however, too much stress must not be placed on the new joint, as it can possibly damage the new knee. While most patients achieve full independence by six weeks, some pain, stiffness and warmth is normal and expected even months after the surgery.
- Driving usually resumes within three to six weeks after surgery.
- The surgeon will approve when it is okay to return to regular exercises and sports. In the meantime, walking, swimming after the wound is healed, and performing low impact activities such as light tennis, bicycling or golfing are okay. High impact activities are discouraged as they may decrease the longevity of the knee replacement, as well as deep bending.
- Any sleeping position is fine.
- The return to work is dependent upon multiple factors, including the type of work duties, extensiveness of surgery and recovery rate. Return to work may take several weeks to a few months, and the doctor will approve when work may be resumed.
- The doctor will determine when it is safe to resume sexual activity, usually after several weeks post-surgery for most patients.
- Though travel is not restricted, air travel will impact the knee, especially during early healing. Pressure changes and the immobility for extended periods of time may cause swelling and lead to blood clots. Also, metal detectors may be sensitive to the artificial joint.
- With the approval and supervision of a physician, a weight loss program should be started or continued if started prior to surgery. A healthy weight will extend the life of the knee replacement as well as speed the recovery process and lessen pain and pressure on the knee.
Extending the Life of a Total Knee Replacement
As knee replacements can last up to 20 years or longer with proper care, following all pre- and post-surgical instructions, as well as avoiding weight gain, smoking and high-impact activities will all help ensure the maximum lifespan of the artificial joint. Though the knee joint may be replaced again if needed, the results are not as good as with the first replacement.
In the past, many surgeons recommended that younger patients do not undergo a knee replacement until they are older. This was due to the shorter lifespan of the prosthesis. Now, with advances in material sciences, prosthetics last much longer than in the past, and younger patients are now viable candidates.
If you are experiencing pain from knee arthritis and conservative treatment measures are no longer effective, request an appointment with a joint replacement specialist at UOA. We will be able to describe your treatment options and help you determine if a knee replacement is right for you.





