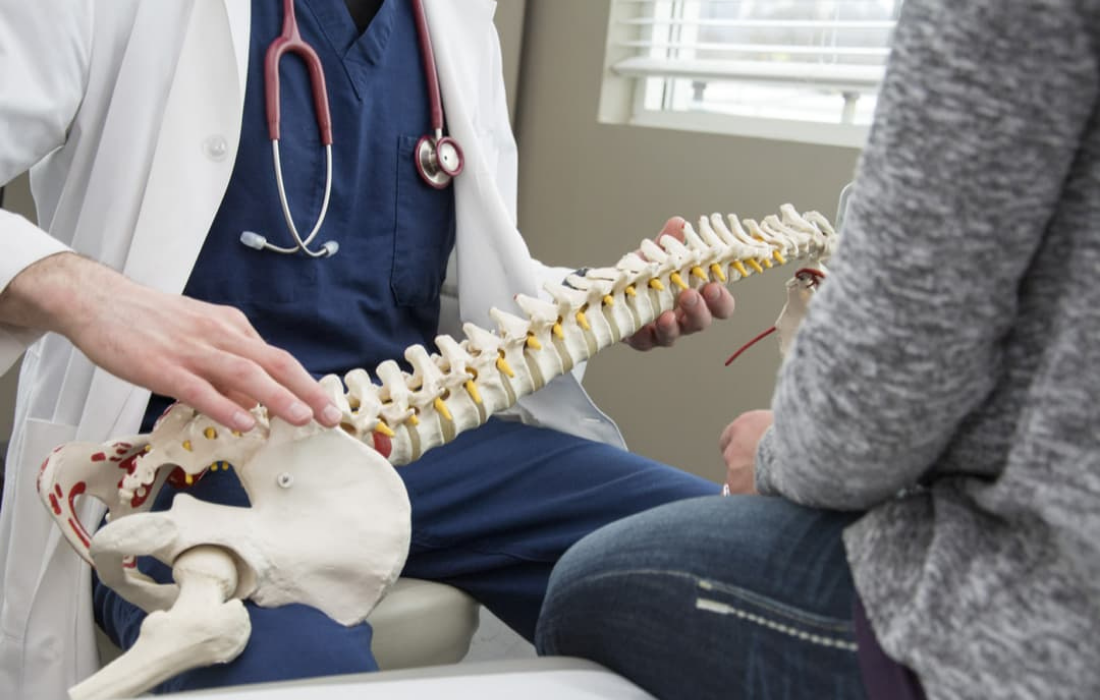
Herniated discs are one of the most common causes of back pain. Between each vertebra is a fibrocartilage disc that cushions the vertebrae and acts as shock absorbers. Whether due to age or injury, sometimes the soft inner layer of the disc 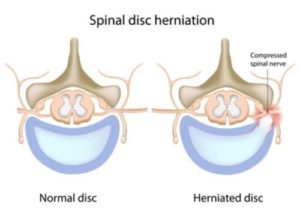 punches through the hard outer layer and creates a bulge.
punches through the hard outer layer and creates a bulge.
Think of a jelly donut that’s been crushed at the bottom of a shopping bag. The donut is the outer disc layer, and the jelly that squirts out is the bulge. If this bulge presses on a nerve root stemming from the spinal cord, the result can cause pain and other symptoms.
Herniated Disc Causes
Herniated discs are more often a chronic injury due to age and wear-and-tear,—most people can’t pinpoint one specific event that led to their symptoms.
Degenerative disc disease is an age-related cause of herniated discs. As people age, their discs dry out (a process called desiccation), making them weaker and more prone to herniation.
Sometimes herniated discs are the direct result of a specific injury. These can range from high energy injuries like car accidents or falls to lower energy injuries from improper lifting or twisting.
Herniated disc risk factors
Factors that make herniated discs more likely include:
- Age
- Physically demanding jobs
- Lifting heavy weights incorrectly (with too little assistance from the leg muscles)
- Smoking, which speeds the desiccation process
- Genetic factors
Herniated Disc Symptoms
Herniated disc symptoms mostly depend on where the herniation in the spine occurs. Disc herniations are more likely to happen in the neck (cervical spine) and lower back (lumbar spine), rather than the mid or upper back (thoracic spine).
Lumbar herniated disc symptoms include:
- Sciatica, a shooting pain that radiates from the buttocks down the leg
- Weakness in the leg or foot
- Lower back pain
- Numbness or tingling in the leg or foot
In rare cases, a long-term herniated disc in the lower back can cause loss of bladder or bowel control. This may be a sign of cauda equina syndrome, which is a medical emergency that needs treatment right away.
A herniated disc in the cervical spine can cause:
- Pain radiating down one arm
- Weakness in one arm
- Numbness or tingling in the arm
- Upper back pain
- Constant headache
Herniated Disc Diagnosis
Most herniated discs can be diagnosed by a healthcare provider with a physical exam and medical history. A doctor will be looking for signs of acute injury, how long symptoms have lasted and any lifestyle risk factors.
During a physical exam, the doctor will often perform a neurological exam to check for symptoms such as numbness and weakness, which indicate a problem with nerves. The doctor may also check the back for any signs of tenderness or inflammation, and move the legs or arms in various positions to see if any trigger pain.
A magnetic resonance imaging (MRI) scan may help confirm a herniated disc diagnosis. Herniated discs will not show up on X-rays, but MRIs are useful for depicting problems with soft tissue such as intervertebral discs.
Herniated Disc Treatment
The majority of herniated discs resolve on their own with no surgery necessary. Conservative, nonoperative treatment aimed at managing pain and other symptoms is usually the first method of treatment and often all that’s necessary.
 Conservative treatment can include:
Conservative treatment can include:
- Rest
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
- Physical therapy
- Corticosteroid injections
If pain and other symptoms persist, surgery may be necessary. A laminectomy may be helpful for a herniated disc. Laminectomies remove the back of a vertebra called the lamina, which makes more room in the spinal canal and relieves pressure on the nerve.
Another surgical option may be a discectomy or microdiscectomy (micro– for the microscope glasses called loupes the surgeon uses). This is when a surgeon removes the herniated portion of the disc that is compressing the nerve.
There is a special procedure for cervical herniations known as anterior cervical discectomy and fusion (ACDF). A surgeon accesses the disc from the front of the throat (an anterior approach) rather than the back. The surgeon performs a discectomy and also fuses the affected vertebra with the one above it to ensure the spine is aligned properly and to eliminate potentially painful spinal movement.
If you are troubled by back, neck, leg or arm pain and think you may have a herniated disc, request an appointment with one of UOA’s spine experts. They will be able to diagnose the source of your pain and recommend a treatment plan that’s right for you.