Lumbar Disc Herniation
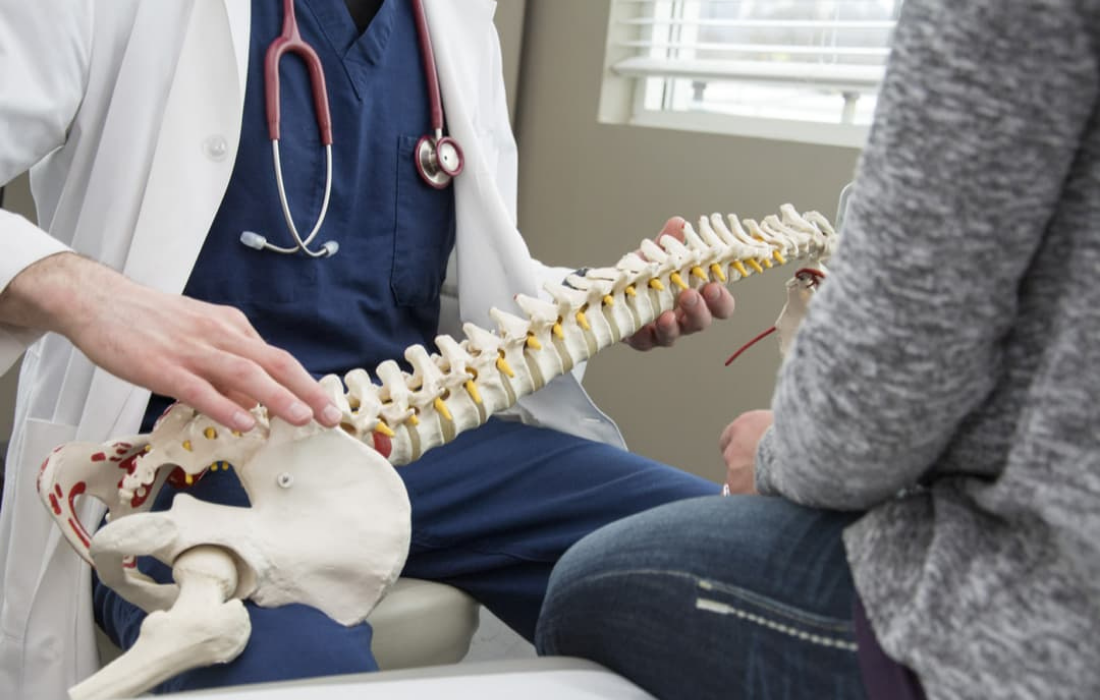
Lumbar Disc Herniation is most common in patients in their thirties and forties. This condition often occurs as a result of degenerating discs in the spine. Discs are located between the vertebrae and serve as cushions between the bones. When the disc begins to degenerate, the inner core can bulge or herniate into the spinal canal or nerve tunnels. A herniated disc can put pressure on a spinal nerve and produce significant pain. The patient can present with back pain or with pain radiating into the buttock or leg. This referred pain is termed radiculopathy, or “sciatica.” At times, the referred pain can be extremely uncomfortable or even debilitating.
Patients with a lumbar disc herniation can also develop weakness and numbness or tingling in the legs.
Symptoms
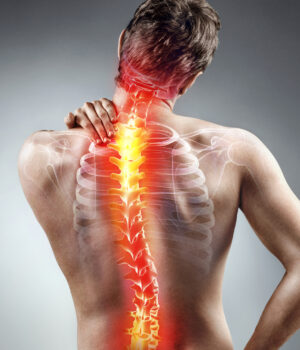
Back pain
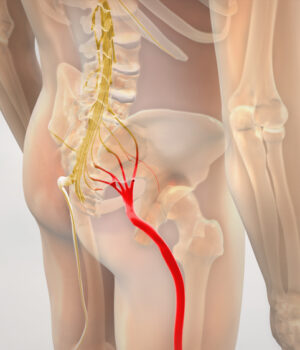
Sciatica

Weakness or numbness of legs
Treatment
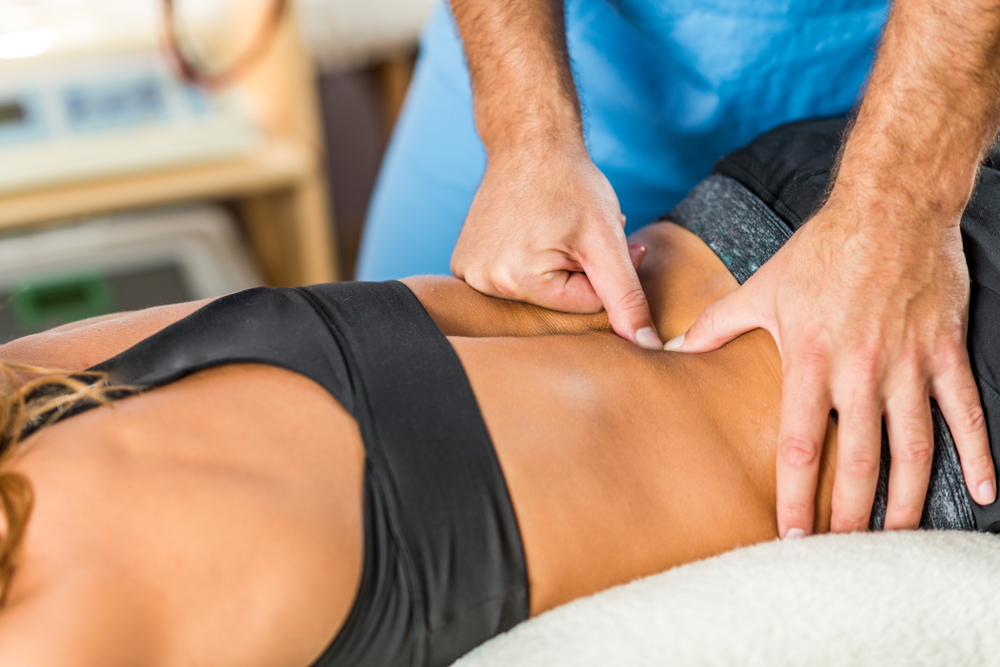
Treatment for herniated discs varies based on location and severity. Many people have bulging or herniated discs without noticing or experiencing pain. Many patients with pain from a herniated disc will improve without surgery. Doctors recommend relative rest and the use of anti-inflammatory medication, muscle relaxants, or oral steroids to help provide relief for patients experiencing severe pain. Physical therapy is often prescribed to strengthen the muscles that support the spine making it less prone to injury. Injections of steroid medication into the spine around the nerves are another non-surgical option. Physicians inject steroid medication into the epidural space or around the irritated nerve root.
Surgery is reserved for patients who fail to improve the nonsurgical methods discussed above and in patients who are experiencing persistent disabling pain or progressive and significant weakness. The surgery to treat a disc herniation is usually a microdiscectomy. This removes the herniated disc and eliminates the pressure on the surrounding nerves.