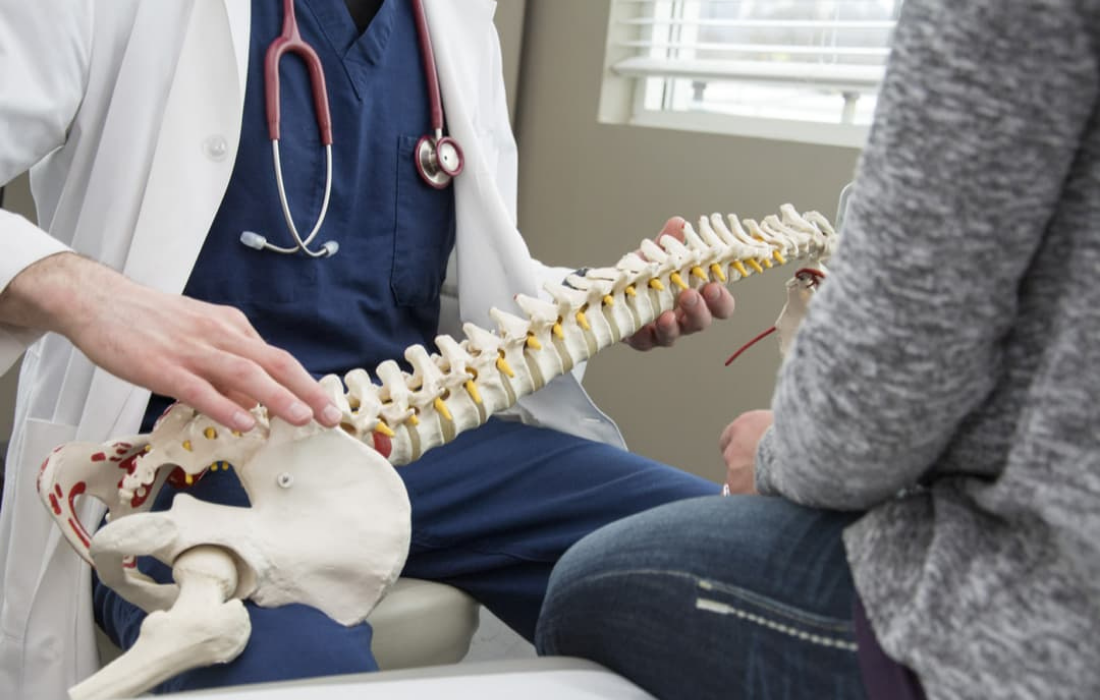
Spinal stenosis is a narrowing of the spaces in the spine, resulting in pressure on the spinal cord and nerves. The narrowing can occur anywhere along the spine, but is typically found in lumbar (low back) and cervical (neck) region. In some instances, spinal stenosis can result in myelopathy, an injury to the spinal cord due to compression.
Causes
Typically, spinal stenosis is due to wear-and-tear from osteoarthritis, including the formation of bone spurs (bony overgrowths). Osteoarthritis is the most common form of arthritis and occurs when the cartilage that protects the ends of the bones wears down over time.
Other causes of spinal stenosis can include:
- Herniated discs that press on the spinal cord or nerves
- Injuries to the spine, such as from a car accident, that can cause displaced bone or swelling
- Spinal tumors that can form in the space between the vertebrae and spinal cord or within the membranes that cover the spinal cord
- Thickened ligaments that can bulge into the spinal canal
- Congenital deformities, such as scoliosis
Symptoms
With spinal stenosis, symptoms often appear gradually and slowly worsen over the course of time. They also vary depending on the location of the stenosis.
Symptoms of cervical stenosis include:
- Bladder or bowel dysfunction (in severe cases)
- Difficulty with balance and walking
- Neck pain
- Tingling, numbness or weakness in the upper or lower extremities
Symptoms of lumbar stenosis include:
- Back pain
- Cramping or pain in one or both legs after standing for a while or walking, which improves when sitting or bending forward
- Tingling, weakness or numbness in the leg or foot
Diagnosis
After taking a medical history and conducting a physical examination, a physician may have some imaging tests done to confirm a diagnosis. These include:
- A computed tomography (CT) scan in the event an MRI can’t be performed that can detect herniated discs, bone spurs and tumors as well as damage to the spinal cord and nerves
- A magnetic resonance imaging (MRI) scan to look for damage to the discs and ligaments, as well as any tumors and where pressure is occurring along the spinal cord
- An X-ray to reveal any bony changes to the spine, such as bone spurs
Treatment
Treatment for spinal stenosis depends on the severity of the symptoms and the location of the stenosis. If symptoms are mild or lacking, a physician may recommend simply monitoring the condition and recommend some self-care tips patients can incorporate into their daily activities.
Should self-care fail or symptoms worsen, other recommended treatments can include:
- Medications, such as over-the-counter (OTC) pain relievers (e.g., naproxen sodium, ibuprofen, etc.), certain antidepressants, certain anti-seizure drugs or opioids
- Physical therapy to build up muscle strength, maintain flexibility in the spine and improve balance
- Steroid injections to reduce inflammation around the pinched nerves and relieve some of the pain
- Percutaneous image-guided lumbar decompression (PILD), which utilizes needle-like instruments to remove portions of thickened ligaments to free up space in spinal canal and relieve pressure on a nerve root
Surgery
If all other methods of treatment have failed in relieving symptoms, surgery for spinal stenosis may be considered to create more space in the spinal canal. Surgical procedures include:
- Laminectomy to remove all of the lamina, the protective cover of the spinal canal (may require placement of hardware or bone graft to reinforce the spine)
- Laminotomy to remove a portion of the lamina
- Laminoplasty (performed only on the cervical spine), which opens up a space in the spinal canal by creating a hinge on the lamina so metal hardware can bridge the gap in the canal